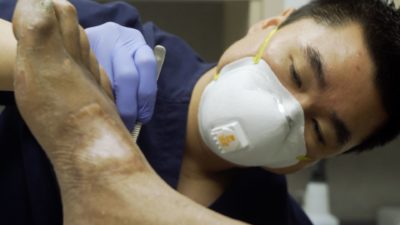
 Wound care is critical for everyone, including diabetic patients where it is most crital.
Wound care is critical for everyone, including diabetic patients where it is most crital.
Wounds and ulcers that will not heal can lead to serious complications. Getting proper treatment from our experienced podiatrists is critical. We use state-of-the-art tools, along with advanced techniques to provide you with the best possible solutions. Patients with diabetes should take extra care of wounds to reduce the risk of infection and amputation, improve function and quality of life.
The primary goal in the treatment of foot ulcers is to obtain healing as soon as possible. The faster the healing process begins, the less chance for an infection. Key factors in the immediate attention to the treatment of a diabetic foot ulcer include:
- Prevention of infection
- Taking the pressure off the area, called “off-loading”
- Removing dead skin and tissue, called “debridement”
- Applying medication or dressings to the ulcer
- Managing blood glucose and other health problems
The best way to treat a foot ulcer is to prevent its development in the first place. It is important to see a podiatrist on a regular basis. Our podiatrist can determine if you are at high risk for developing a foot ulcer and implement strategies for prevention. Again, this is highly important if you are diabetic. Patients at high risk often develop these symptoms:
- Neuropathy
- Poor circulation
- A foot deformity (e.g., bunion, hammertoe)
- Uncontrolled blood sugar
- History of a previous foot ulceration
Prevention of an ulcer from becoming infected, it is important to:
- Keep blood glucose levels under tight control;
- Keep the ulcer clean and bandaged;
- Cleanse the wound daily, using a wound dressing or bandage; and
- Avoid walking barefoot
- Avoid getting wet in a shower
- Wash separately as bacteria can travel from other parts of the body
Reducing risk factors will also help prevent or manage foot ulcers, such as:
- Smoking
- Alcohol
- High cholesterol
- Elevated blood glucose
- Proper socks and shoes
It is also important to learn how to check your feet to find potential problems as early as possible. Our podiatrist conducts diabetic foot exams on every diabetic patient. Some things you can do at home include:
- Inspect the soles of your feet and include looking between the toes
- Look for cuts, bruises, cracks, blisters, and redness
- Any signs of a wound should result in an immediate visit to a podiatrist
For optimum healing of ulcers, you may be asked to wear special footwear, brace, castings, or use a wheelchair or crutches. These devices will reduce the pressure and irritation of the ulcer and help speed the healing process.
Wounds and ulcers heal faster, with a lower risk of infection, if they are kept covered and moist. The use of full-strength betadine, hydrogen peroxide, whirlpools, and soaking is NOT recommended, as these practices could lead to further complications. Please see a podiatrist before administering self-care.
Appropriate wound management includes the use of dressings and topically-applied medications. Products range from normal saline to growth factors, ulcer dressings, and skin grafts that have been shown to be highly effective in healing foot ulcers.
For a wound to heal, there must be adequate circulation to the ulcerated area. Our podiatrists can determine circulation levels with noninvasive tests.
As previously stated, controlling blood glucose is of the utmost importance during the treatment of a diabetic foot ulcer. Working closely with a medical doctor or endocrinologist to control blood glucose will enhance healing and reduce the risk of complications.
Healing time depends on a variety of factors, such as wound size and location, pressure on the wound from walking or standing, swelling, circulation, blood glucose levels, wound care, and what is being applied to the wound. Healing may occur within weeks or require several months.
Conditions treated
- Complications of diabetes
- Complications of vascular disease
- Complications of neuropathy
- Prolonged wear of ill-fitting shoes
- Long periods of bed rest or immobility
- Injuries that break the skin
- Skin infections
To request an exam of your wound or feet, please reach out to us through our appointment request form and we will be sure to help you get started with the right care your feet need.